Miscarriage is defined as the loss of a pregnancy before it has reached 20 weeks’ gestation. If a loss of pregnancy occurs after 20 weeks, it is known as a stillbirth. Miscarriages often occur without any obvious cause. When a pregnancy ends prematurely, it can be very distressing; however, counselling and support are available.…
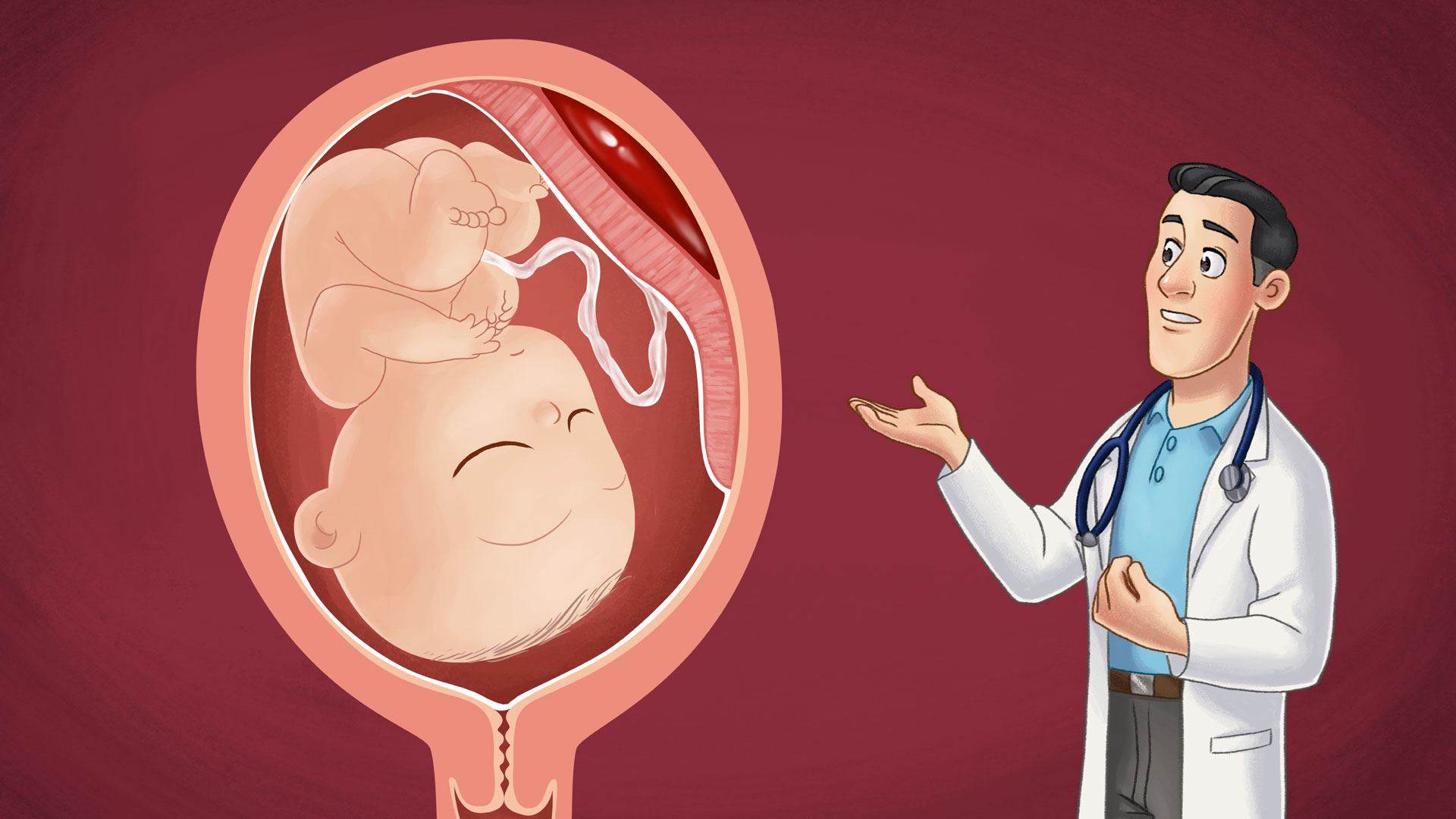
Placental abruption
What is placental abruption?
A placental abruption occurs in pregnant women when the placenta detaches from the wall of the uterus before the baby has been born. It is a serious condition that can threaten the life of both the mother and the baby.
Placental abruption is known by a number of other names, including placental abruptio and abruptio placenta. It occurs in around 1% of pregnancies and is the leading cause of vaginal bleeding in the latter half of pregnancy.
Because it can cause heavy bleeding in the mother and stop vital nutrients and oxygen reaching the baby, placental abruption requires urgent medical assessment and treatment.
Placenta
The organ that forms within the uterus of a pregnant woman to provide the fetus with nourishment from the blood supply of the mother.
Uterus
The hollow organ of the female reproductive system that is responsible for the development of the embryo and fetus during pregnancy. Also known as the womb.
Antepartum haemorrhage (APH) including placenta praevia abruption and vasa praevia. 3 Centres Collaboration. Accessed August 18 2014 from
External linkWhat is the placenta?
The placenta grows inside the uterus and plays a vital role during pregnancy.
The placenta:
- Transfers nutrients and oxygen from the mother's blood supply to the baby;
- Removes waste products from the baby's blood;
- Is attached to the baby by the umbilical cord and to the mother via part of the uterus wall, and;
- Normally, the placenta detaches from the uterus just after the birth of the baby, which allows it to also be delivered (called the afterbirth).
Placenta
The organ that forms within the uterus of a pregnant woman to provide the fetus with nourishment from the blood supply of the mother.
Uterus
The hollow organ of the female reproductive system that is responsible for the development of the embryo and fetus during pregnancy. Also known as the womb.
Antepartum haemorrhage (APH) including placenta praevia abruption and vasa praevia. 3 Centres Collaboration. Accessed August 18 2014 from
External linkCauses
If the placenta detaches either partially or completely from the wall of the uterus before birth, this is called a placental abruption. It can lead to damage to the blood vessels in the wall of the uterus, resulting in bleeding, which can present as vaginal bleeding. However, if the blood clots between the uterus and placenta (called a retroplacental clot), the bleeding will largely be concealed - there may be little or no sign of it. Placental abruption can result in bleeding that is either visible or invisible.
Placental abruption can result in bleeding that is either visible or invisible.
Depending on how complete the detachment of the placenta from the uterus, the baby may no longer receive enough nutrients and oxygen to survive.
While in most cases it is not known what causes the placental abruption to occur, there are two known direct causes:
Trauma
Trauma, such as that which can occur in a car accident causing a blow to the abdomen or a fall, can lead to a placental abruption. It is important to note that a placental abruption can occur without any direct trauma or contact to the abdomen and symptoms can take hours or days to show.
Sudden reduction of uterine size
A sudden loss of amniotic fluid (the fluid that surrounds the baby within the amniotic membranes), which can occur when the waters break during labor, can create a vacuum-like effect that can pull the placenta away from the wall of the uterus and result in bleeding.
Abdomen
The part of the body that lies between the chest and the pelvis.
Placenta
The organ that forms within the uterus of a pregnant woman to provide the fetus with nourishment from the blood supply of the mother.
Uterus
The hollow organ of the female reproductive system that is responsible for the development of the embryo and fetus during pregnancy. Also known as the womb.
Clot
The thickened or solid mass formed from a liquid, such as blood. Blood clots normally form at an injury site to prevent further blood loss.
Antepartum haemorrhage (APH) including placenta praevia abruption and vasa praevia. 3 Centres Collaboration. Accessed August 18 2014 from
External linkRisk factors
A range of factors can increase the risk of a woman having a placental abruption.
Medical conditions
Medical conditions that can increase the risk of an abruption include:
- High blood pressure (hypertension);
- Pre-eclampsia;
- Conditions causing problems with blood clotting;
- Diabetes;
- Inflammation of the amniotic membranes (chorioamnionitis);
- Uterine fibroids, and;
- Scarring of the uterus from previous surgery.
Pregnancy factors
A woman's risk of placental abruption is greater:
- The more pregnancies she has had;
- The older she is;
- If she is having a multiple pregnancy (twins or more), and;
- If she has too much amniotic fluid (polyhydramnios).
Medical procedures
Procedures such as amniocentesis and amnioreduction can slightly increase the risk of a placental abruption.
Amniocentesis is a test done during pregnancy in which a needle is inserted through the mother's abdomen and into the uterus in order to obtain a sample of amniotic fluid. Tests using the amniotic fluid can identify a range of medical conditions in the baby, such as Down syndrome.
In amnioreduction, the needle is used to remove excess amniotic fluid because too much has accumulated in the amniotic sac.
Other risk factors
A woman's risk of placental abruption is greater if, during pregnancy, she:
- Smokes;
- Drinks alcohol, and/or;
- Uses recreational drugs such as, cocaine and methamphetamines.
Abdomen
The part of the body that lies between the chest and the pelvis.
Diabetes
A metabolic disorder that is caused by problems with insulin secretion and regulation and which is characterized by high blood sugar levels. Also known as diabetes mellitus.
Uterine fibroids
Abnormal growths that develop from the muscle in the walls of the uterus. They are not cancerous, however, they can cause a range of symptoms including pain, pressure in the pelvis and heavy menstrual bleeding.
Uterus
The hollow organ of the female reproductive system that is responsible for the development of the embryo and fetus during pregnancy. Also known as the womb.
Antepartum haemorrhage (APH) including placenta praevia abruption and vasa praevia. 3 Centres Collaboration. Accessed August 18 2014 from
External linkTypes
Placental abruptions can be partial or complete.
During a partial abruption, some of the placenta is still attached to the wall of the uterus. In less serious cases, the baby is still able to get enough oxygen and nutrients for the pregnancy to continue, however, precautions may need to be taken to prevent further damage to the placenta.
Following a complete abruption, the placenta detaches entirely from the wall of the uterus. It is a very serious, life-threatening condition for both mother and baby. If it occurs, emergency treatment (a caesarean section) is required to deliver the baby as soon as possible.
Placenta
The organ that forms within the uterus of a pregnant woman to provide the fetus with nourishment from the blood supply of the mother.
Uterus
The hollow organ of the female reproductive system that is responsible for the development of the embryo and fetus during pregnancy. Also known as the womb.
Antepartum haemorrhage (APH) including placenta praevia abruption and vasa praevia. 3 Centres Collaboration. Accessed August 18 2014 from
External linkSigns and symptoms
Symptoms of a placental abruption can include:
- Vaginal bleeding, although a placental abruption can also occur with little or no visible bleeding;
- Continuous pain in the abdomen that can be severe. However, a placental abruption can occur without pain;
- Continuous back pain, and;
- Very frequent contractions of the uterus.
A doctor's examination may find:
- The uterus is hard and tender when palpated (pressed with the hands) over the mother's abdomen, and;
- Signs of fetal distress, such as an abnormal heartbeat.
Abdomen
The part of the body that lies between the chest and the pelvis.
Uterus
The hollow organ of the female reproductive system that is responsible for the development of the embryo and fetus during pregnancy. Also known as the womb.
Antepartum haemorrhage (APH) including placenta praevia abruption and vasa praevia. 3 Centres Collaboration. Accessed August 18 2014 from
External linkMethods for diagnosis
The symptoms of a placental abruption can be similar to other conditions that can occur in the latter half of pregnancy, including pre-eclampsia and low-lying placenta.
Your doctor will ask you about your symptoms, your medical history and whether or not you have experienced any trauma.
Other tests may include:
- A pelvic exam to view the vagina and cervix;
- An ultrasound to check the placenta. A retroplacental clot may be visible in an ultrasound, but this is not always the case;
- Monitoring the baby for signs of distress, including measuring fetal heart rate, and;
- Blood tests.
Blood tests can be used to:
- Measure the mother's hemoglobin levels;
- Detect signs of blood-clotting abnormalities (tests include measuring fibrinogen level and prothrombin time), and;
- Detect the baby's hemoglobin in the mother's bloodstream (the Kleihauer-Betke test).
 Your doctor will discuss the various methods for diagnosis of placental abruption.
Your doctor will discuss the various methods for diagnosis of placental abruption.
Cervix
The lower part of the uterus, leading out into the vagina.
Hemoglobin
A protein molecule found in red blood cells, crucial for transporting oxygen to the body's cells.
Placenta
The organ that forms within the uterus of a pregnant woman to provide the fetus with nourishment from the blood supply of the mother.
Clot
The thickened or solid mass formed from a liquid, such as blood. Blood clots normally form at an injury site to prevent further blood loss.
Prothrombin
An inactive form of the thrombin enzyme which, once activated, is important for the formation of blood clots that help stop bleeding.
Antepartum haemorrhage (APH) including placenta praevia abruption and vasa praevia. 3 Centres Collaboration. Accessed August 18 2014 from
External linkTypes of treatment
Treatment for a placental abruption can vary depending on a number of factors, such as:
- The severity of the placental abruption and bleeding;
- The pregnancy stage during which the placental abruption occurs, and;
- Whether the baby is showing signs of distress.
In mild cases, where the bleeding stops and the baby is not showing signs of distress, conservative management may be recommended. This is particularly the case earlier in pregnancy, when the baby is not ready to be born. This may mean resting at home, with regular check-ups, or you may be recommended to remain in hospital to be monitored until the delivery of the baby.
If the placental abruption is more severe, a blood transfusion or intravenous (IV) fluids may be recommended for the mother. Your doctors may also recommend bringing forward the delivery of your baby. This is particularly the case if the placental abruption occurs later in pregnancy. Depending on your circumstances, labor may be induced and a vaginal delivery may be possible, or you may be recommended to have a caesarean section.
If delivery is planned and the baby will be born significantly prematurely, medications such as magnesium sulfate and corticosteroids may be recommended to be taken by the mother to help protect the baby from complications related to premature birth.
If the life of the mother or baby is at risk, emergency caesarean section, performed as soon as possible, will usually be recommended.
Corticosteroids
A medication that resembles the cortisol hormone produced in the brain. It is used as an anti-inflammatory medication.
Antepartum haemorrhage (APH) including placenta praevia abruption and vasa praevia. 3 Centres Collaboration. Accessed August 18 2014 from
External linkPotential complications
Excessive hemorrhage and shock
When too much blood is lost, it can lead to a condition called shock, in which there is not enough blood flow around the body. In this situation, organs in the body do not receive enough oxygen and this can lead to damage and death.
A placental abruption can increase the risk of excessive bleeding from the uterus following the delivery of the baby. There are a range of surgical techniques to control bleeding. If these are not successful, a hysterectomy (removal of the uterus) may be needed to save the life of the mother.
Disseminated intravascular coagulation
Disseminated intravascular coagulation (DIC) is a condition in which small blood clots develop in blood vessels throughout the body. These clots can block blood flow and oxygen to vital organs. They can also use up much of the body's supply of platelets and substances that promote clotting in the blood. This can then lead to an increased risk of internal bleeding (such as in the uterus) that is excessive because it is unable to clot normally.
DIC can be life-threatening. Women who are suspected of having a placental abruption will generally have a blood test to measure clotting factors in their blood and determine whether they are at risk of DIC.
Rhesus disease
Rhesus disease occurs when a mother's antibodies damage the developing baby's blood cells. It can lead to the baby developing anemia and jaundice.
Rhesus disease can develop when the following three things occur:
- The mother has a Rhesus negative blood type;
- The baby has a Rhesus positive blood type, and;
- The mother has been previously exposed to Rhesus positive blood (this is called rhesus sensitization).
In a placental abruption, blood from the baby can pass into the mother's bloodstream, which can lead to Rhesus sensitization. Tests of the mother's blood, such as the Kleihauer-Betke test, can detect the presence of the baby's blood in the mother's bloodstream.
Rhesus disease may affect the baby in the present pregnancy or in later pregnancies.
Women who have a Rhesus negative blood type may be recommended to have an injection of anti-D immunoglobulin following a placental abruption. This can remove the baby's blood cells from the mother's bloodstream and help to prevent sensitization.
Stillbirth of the baby
A placental abruption can lead to damage to or death of the baby.
If the birth is premature, the baby may also be at risk of complications related to prematurity.
Anemia
A deficiency in red blood cells or hemoglobin in the body.
Jaundice
A yellowing of the skin, the whites of the eyes and the mucous membranes, due to an accumulation of bilirubin in the blood. Often a symptom of liver problems.
Platelets
Small blood cells found in the blood that are essential for clotting to occur.
Uterus
The hollow organ of the female reproductive system that is responsible for the development of the embryo and fetus during pregnancy. Also known as the womb.
Clot
The thickened or solid mass formed from a liquid, such as blood. Blood clots normally form at an injury site to prevent further blood loss.
Antepartum haemorrhage (APH) including placenta praevia abruption and vasa praevia. 3 Centres Collaboration. Accessed August 18 2014 from
External linkPrognosis
Severe placental abruption can be life-threatening. However, prompt treatment can help to save the lives of both mother and baby.
Antepartum haemorrhage (APH) including placenta praevia abruption and vasa praevia. 3 Centres Collaboration. Accessed August 18 2014 from
External linkPrevention
There are things you can do to help reduce your risk of having a placental abruption.
As part of your antenatal care, work with your doctor or midwife to make sure:
- Your blood pressure is under control;
- Any medical conditions, such as diabetes or pre-eclampsia are appropriately treated, and;
- Your healthcare professionals know if you have had a placental abruption in a previous pregnancy or any other problems that might increase your risk.
 Measuring your blood pressure helps to monitor your well-being during pregnancy.
Measuring your blood pressure helps to monitor your well-being during pregnancy. You can also:
- Avoid alcohol, stop smoking and using recreational drugs and medications that have not been prescribed by your doctor during pregnancy, and;
- Take sensible steps to avoid trauma, such as wearing a seatbelt when driving and avoiding tripping hazards or things that could make you fall.
Diabetes
A metabolic disorder that is caused by problems with insulin secretion and regulation and which is characterized by high blood sugar levels. Also known as diabetes mellitus.
Antepartum haemorrhage (APH) including placenta praevia abruption and vasa praevia. 3 Centres Collaboration. Accessed August 18 2014 from
External link





