The average pregnancy is counted as 40 weeks, starting from the first day of the mother’s last period. Pregnancy is divided into three trimesters, with different stages in each. The development of a pregnancy can be followed week by week, but it’s important to remember the experience varies for every mother and baby.…
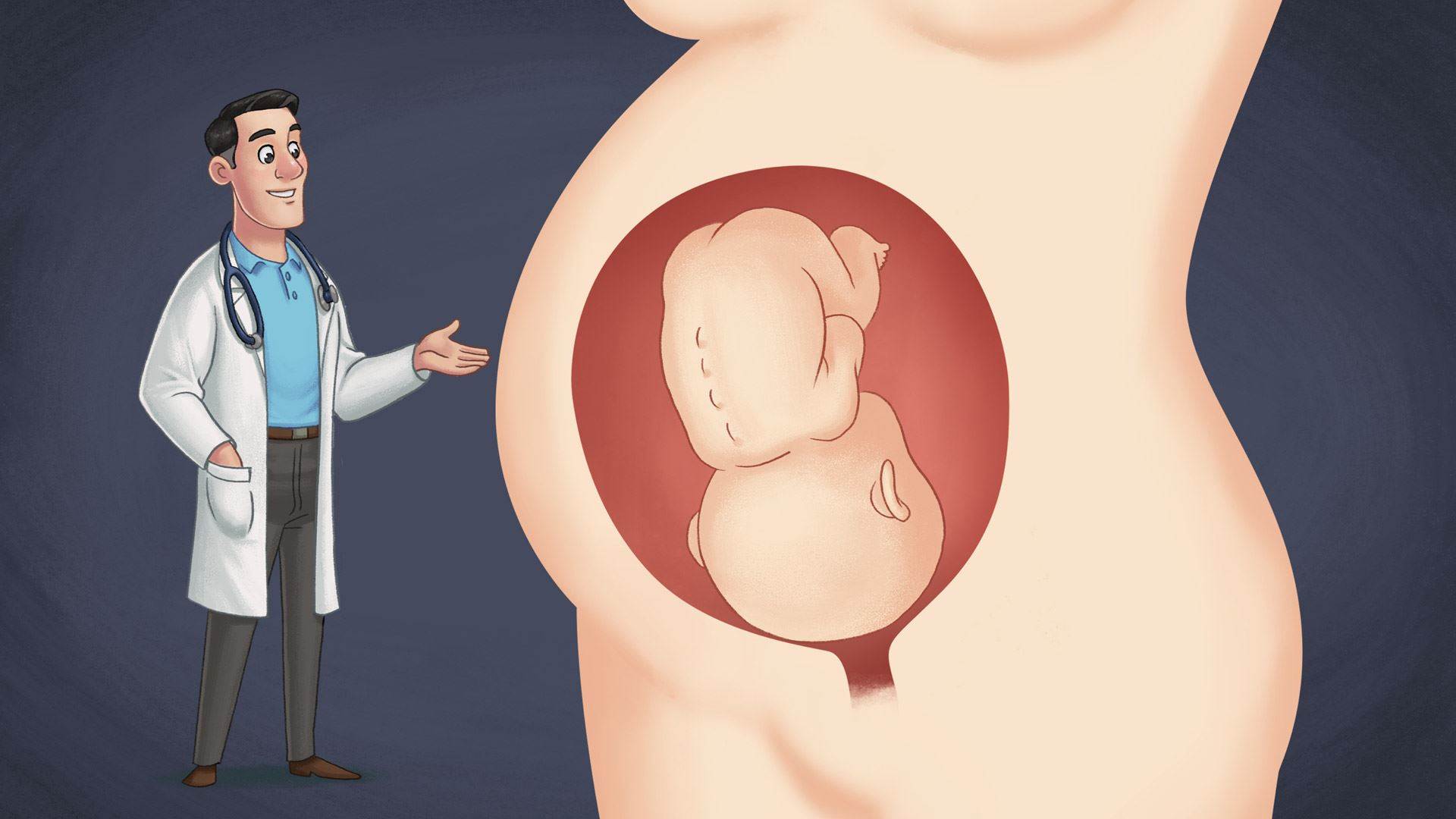
Fetal position during pregnancy
Fetal position during pregnancy
When a fetus starts developing in the uterus, it is very small and has a lot of room. It floats around and changes position freely.
As a fetus grows, it starts filling up the available space inside the uterus. Most fetuses spend some time lying sideways in the uterus. At 28 weeks' gestation, one in five of every fetuses are in the breech position (head up, buttocks down). Eventually, however - normally at around 36 weeks - the majority of babies finally settle with their head down toward the mother's vagina. When childbirth begins, the baby's head is first to emerge from the birth canal, followed by the rest of the body.
In a few cases, the fetus is not facing this way. This might lead to a complicated birth process and may pose risks to the baby and mother. In these cases, a caesarean section (C-section) may be considered to help deliver the baby.
If your baby has not settled into a headfirst position by week 32, follow-up is recommended. Around week 36, an ultrasound scan can check the fetal position and your doctor or midwife will explain the options for the final weeks of your pregnancy.
Fetus
An unborn human, from the ninth week of pregnancy until birth.
Uterus
The hollow organ of the female reproductive system that is responsible for the development of the embryo and fetus during pregnancy. Also known as the womb.
Gestation
The period of fetal development in the womb from conception to birth.
Risk factors
The chance of incorrect fetal positioning at birth may be increased in certain circumstances, including:
- Preterm labor;
- Multiple births, e.g., twins or triplets;
- Certain fetal medical conditions, such as megacephaly;
- Previous breech birth, and;
- Placental and uterine abnormalities.
Megacephaly
A congenital condition characterized by an abnormally large head.
Methods for diagnosis
The birth position is determined by your doctor or midwife palpating (examining by touch) your abdomen. Ultrasound is used to provide a clear picture of the fetus's position.
Abdomen
The part of the body that lies between the chest and the pelvis.
Fetus
An unborn human, from the ninth week of pregnancy until birth.
Positions
Headfirst
In more than 95% of births, the fetus's head is facing downward towards the mother's vagina. However, this can occur in several ways.
Occiput anterior (OA)
This is the most common and favorable birth position. The baby's head is down near the mother's vagina, with the face directed towards the mother's rear. Its head is also bent down, so the chin is resting against the chest and the feet are crossed.
 The occiput anterior position.
The occiput anterior position. Occiput posterior (OP)
The baby's head is down near the mother's vagina, but the face is directed towards the mother's front. In the weeks leading up to birth, 10-15% of fetuses are in this position, but most of them rotate their body shortly before birth and only 5-6% are born while in this position. The OP position - also known as 'face up' or 'sunny-side up' - may cause a longer and more difficult labor.
 The occiput posterior position.
The occiput posterior position. Occiput transverse (OT)
The baby's head is down near the mother's vagina, with the face towards the mother's side. This is an uncommon position. Forceps or vacuum extraction can be used to rotate to assist birth, if required. A caesarean section may be performed in certain circumstances.
Face and brow presentations
In these rare presentations, the baby is in the normal OA position, but the baby's face is first to enter the birth canal rather than the top of the head. This is due to the chin pointing out rather than resting against the baby's chest. These presentations are usually discovered only once labor has started.
In the face presentation, which occurs once in every 800-900 births, the baby's entire face is first to enter the birth canal. A vaginal examination at the start of labor will reveal this, as your doctor of midwife can feel the features of the face with their fingers. A baby in face presentation can be delivered normally, although there may be difficulties that may raise the need for a C-section. A baby born in face presentation can sometimes sustain bruises to the face, but these generally disappear shortly after birth.
In the brow presentation, which occurs once in every 750-1700 births, it is the baby's forehead that is first to enter the birth canal. This can sometimes make for a more difficult labor and in some cases a C-section may be required.
 Brow and face presentations.
Brow and face presentations.
Compound presentation
Compound (or complex) presentation occurs less than once in every 400-1200 births. In this presentation, a limb (usually an arm or hand) is lying near the birth canal alongside the head. This presentation requires extra care during labor, but the limb will usually slide back during the birth process.
Breech
About 3-4% of babies are in the breech position when labor starts. The baby's buttocks are positioned down near the mother's vagina, while baby's head is facing upwards. There are several variations of the breech position:
- Frank breech - with legs straight up, feet near baby's face;
- Complete breech - with legs bent at the knees and crossed, and;
- Footling (Incomplete) breech - one or both of baby's feet are facing down, and will be the first to emerge from the birth canal.
 The three different types of breech positions.
The three different types of breech positions. Transverse (shoulder presentation)
In this position, the baby is lying sideways with its shoulder resting against the mother's pelvis. As noted above, most fetuses will lie sideways in the uterus at some point in the pregnancy. A fetus who maintains this position up to birth is a rare case, occurring only once in every 200-400 births.
A baby in the transverse position at labor cannot be born by vaginal delivery; a C-section must be performed.
 The transverse position.
The transverse position. Umbilical cord presentation and cord prolapse
In uncommon cases (once every few hundred births), the umbilical cord may be the first to enter the birth canal, below the body (head or buttocks) of the baby. This can be a cause for concern, as the umbilical cord is the baby's lifeline. If the cord is under pressure and is blocked during delivery (normally by the baby's head passing through the birth canal), the baby could be in danger.
The difference between cord presentation and cord prolapse is in relation to when the waters break (when fetal membranes rupture). Cord presentation is when the cord enters the birth canal before the waters break. This gives your doctor time to plan for delivery. Cord prolapse is after the waters break and it is considered an emergency due to the risks to your baby. Most cord prolapses will require an urgent C-section.
 Cord presentation, or prolapse, during delivery.
Cord presentation, or prolapse, during delivery. Fetus
An unborn human, from the ninth week of pregnancy until birth.
Sharmila V. and Babu T.A. (2014) Unusual birth trauma involving face: a completely preventable iatrogenic injury. Journal of Clinical Neonatology 3:120–121.
Gardberg M. Leonova Y. and Laakkonen E. (2011) Malpresentations-impact on mode of delivery. Acta Obstetricia Et Gynecologica Scandinavica 90:540–542.
Zayed F. Amarin Z. Obeidat B. et al. (2008) Face and brow presentation in northern Jordan over a decade of experience. Archives of Gynecology and Obstetrics 278:427–430.
Arya R. Whitworth M. and Johnston T.A. (2007) Abnormal labour: an evidence-based approach. Obstetrics Gynaecology & Reproductive Medicine 17:217–221.
Vitner D. Paltieli Y. Haberman S. et al. (2015) Who delivers in occipito-posterior? A multicentric prospective ultrasound-based measurements of fetal station and position throughout labor in a population of 595 women. Ultrasound in Obstetrics & Gynecology DOI: 10.1002/uog.14821
Verhoeven C.J.M. Rückert M.E.P.F. Opmeer B.C. et al. (2012) Ultrasonographic fetal head position to predict mode of delivery: a systematic review and bivariate meta-analysis. Ultrasound in Obstetrics & Gynecology 40:9–13.
Lenehan P.M. Macdonald D. and Turner M.J. (1986) Face and b-row presentation. Journal of Obstetrics & Gynaecology 7:102–106.
Bhal P.S. Davies N.J. and Chung T. (1998) A population study of face and brow presentation. Journal of Obstetrics & Gynaecology 18:231–235.
Arya R. Whitworth M. and Johnston T.A. (2007) Abnormal labour: an evidence-based approach. Obstetrics Gynaecology & Reproductive Medicine 17:217–221.
Vitner D. Paltieli Y. Haberman S. et al. (2015) Who delivers in occipito-posterior? A multicentric prospective ultrasound-based measurements of fetal station and position throughout labor in a population of 595 women. Ultrasound in Obstetrics & Gynecology DOI: 10.1002/uog.14821
Verhoeven C.J.M. Rückert M.E.P.F. Opmeer B.C. et al. (2012) Ultrasonographic fetal head position to predict mode of delivery: a systematic review and bivariate meta-analysis. Ultrasound in Obstetrics & Gynecology 40:9–13.
Lenehan P.M. Macdonald D. and Turner M.J. (1986) Face and b-row presentation. Journal of Obstetrics & Gynaecology 7:102–106.
Bhal P.S. Davies N.J. and Chung T. (1998) A population study of face and brow presentation. Journal of Obstetrics & Gynaecology 18:231–235.
Gibbs R.S. (2008) Danforth’s Obstetrics and Gynecology. (10th edition) Philadelphia PA: Lippincott Williams & Wilkins.
Simm A. and Woods A. (2004) Fetal malpresentation. Current Obstetrics & Gynaecology 14:231–238.
Gibbs R.S. (2008) Danforth’s Obstetrics and Gynecology. (10th edition) Philadelphia PA: Lippincott Williams & Wilkins.
Simm A. and Woods A. (2004) Fetal malpresentation. Current Obstetrics & Gynaecology 14:231–238.
Murtagh J. MD. (2011). John Murtagh’s General Practice (5th revised edition). North Ryde N.S.W.: McGraw-Hill Publishing.
Simm A. and Woods A. (2004) Fetal malpresentation. Current Obstetrics & Gynaecology 14:231–238.
Zandstra H. and Mertens H.J.M.M. (2013) Improving external cephalic version for foetal breech presentation. Facts Views & Vision in ObGyn 5:85–90.
Hannah M.E. Hannah W.J. Hewson S.A. et al. (2000) Planned caesarean section versus planned vaginal birth for breech presentation at term: a randomised multicentre trial. The Lancet 356:1375–1383.
Gibbs R.S. (2008) Danforth’s Obstetrics and Gynecology. (10th edition) Philadelphia PA: Lippincott Williams & Wilkins.
Murtagh J. MD. (2011). John Murtagh’s General Practice (5th revised edition). North Ryde N.S.W.: McGraw-Hill Publishing.
Simm A. and Woods A. (2004) Fetal malpresentation. Current Obstetrics & Gynaecology 14:231–238.
Types of treatment
If your baby is still incorrectly positioned by the third trimester, some things can be done to guide them into the correct position. Some of these methods will only be performed by a medical professional, others you can try yourself, but it is highly advisable that you consult with your doctor beforehand.
Methods can include:
Before labor
External cephalic version
External cephalic version (ECV) is a medical procedure and can be attempted between 32-37 weeks of pregnancy. Your doctor will place their hands over your abdomen, with one hand over your baby's head and the other on its buttocks, and coax the baby's body toward the correct position. Your doctor will monitor the baby's heart rate using a fetal heart rate monitor, and will often use ultrasound to get a clear picture of the fetal position, the uterus and the amount of amniotic fluid in it.
The success rate of external cephalic version varies (30-61%) and depends on the experience of the doctor performing it. Generally, the method works about half the time.
During labor
If the baby is still in a non-optimal position when labor starts, there are several options your doctor or midwife can consider:
- Internal version - during labor, the birth canal expands and makes the uterus more accessible. Your doctor can then reach inside and attempt to reposition the baby headfirst;
- Breech birth - this can be a safe procedure under certain conditions. If the baby is healthy and full-term, the mother's pelvis is wide and the labor normal, breech birth can be considered, and;
- Caesarean section - if the baby is still maintaining an incorrect posture and breech birth is not recommended, a caesarean section will most often be performed.
Abdomen
The part of the body that lies between the chest and the pelvis.
Amniotic fluid
The fluid surrounding and protecting the fetus inside the uterus during pregnancy.
Pelvis
The bony structure in the lower part of the body trunk that connects the base of the spine to the legs. The pelvis protects important organs, such as the bladder and bowel (and in women, the uterus), and anchors thigh and abdominal muscles.
Trimester
One third of a period of time. Often used to describe the three stages of pregnancy, in which each trimester is about three months long.
Uterus
The hollow organ of the female reproductive system that is responsible for the development of the embryo and fetus during pregnancy. Also known as the womb.
Zandstra H. and Mertens H.J.M.M. (2013) Improving external cephalic version for foetal breech presentation. Facts Views & Vision in ObGyn 5:85–90.
Chamberlain G. and Steer P. (1999) Unusual presentations and positions and multiple pregnancy. BMJ 318:1192–1194.






