Psoriasis: Unravelling Symptoms, Triggers, and Lifestyle Strategies
Let’s take a look at the intricacies of psoriasis, a challenging skin condition that extends beyond the surface. This comprehensive guide aims to provide a deeper understanding of psoriasis, offering insights that extend beyond standard information sources.
What is the main cause of psoriasis?
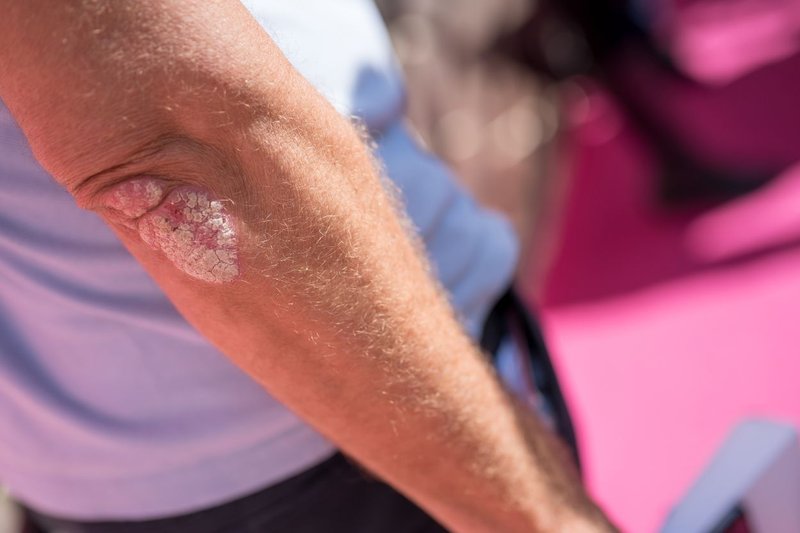
Psoriasis is a chronic autoimmune condition characterised by the rapid growth of skin cells, resulting in the formation of thick, red patches with silvery scales. The condition most commonly appears on the knees, elbows, scalp and lower back, but can develop anywhere.
While the exact cause of psoriasis remains unclear, it is believed to result from a combination of genetic, environmental, and immune system factors.
Genetics play a significant role in psoriasis, with approximately one-third of individuals affected having a family history of the condition. Specific genetic variants associated with psoriasis affect the immune system's regulation of skin cell growth, leading to inflammation and abnormal skin cell proliferation.
Environmental factors such as stress, infections, injury to the skin, and certain medications can trigger or exacerbate psoriasis symptoms in susceptible individuals. Additionally, lifestyle factors including smoking, excessive alcohol consumption, and obesity have been linked to an increased risk of developing psoriasis or worsening existing symptoms.
While psoriasis cannot be cured, various treatments are available to manage symptoms and improve quality of life. These may include topical treatments such as corticosteroids, phototherapy, oral medications, and biologic agents that target specific components of the immune system involved in psoriasis.

There are several types of psoriasis:
Plaque psoriasis
Also known as psoriasis vulgaris, this is the most common type of psoriasis, accounting for around 80% of all cases. Plaque psoriasis usually appears as raised, inflamed, red patches - called plaques - covered by silvery-white scales. It often develops on the scalp, knees, elbows and lower back.
Guttate psoriasis
Guttate psoriasis often occurs in children or young adults and appears as small red spots on the abdomen, arms and legs. These spots are usually not as thick as the patches that develop in plaque psoriasis. Although the rate of guttate psoriasis is quite low, it is still the second-most common type of psoriasis.
Nail psoriasis
Psoriasis of the fingernails and toenails causes discolouration, abnormal nail growth and a pitted appearance. The nails may also become loose, separate from the nail bed, or crumble.
Scalp psoriasis
This type of psoriasis appears on the scalp as red, itchy, silvery scales that may flake off when the hair is brushed or combed.
Inverse psoriasis
Inverse psoriasis is characterised by smooth, red patches of skin without scaly plaques. As the condition is aggravated by sweat and friction, symptoms typically affect the groin, genitals, armpits, the skin under the breasts and anywhere else where skin can rub against itself. It also can arise in the skin folds of people who are overweight. Inverse psoriasis is also known as flexural psoriasis or intertriginous psoriasis.
Pustular psoriasis
This type of psoriasis is quite uncommon and usually seen in adults. The condition is characterised by white, pus-filled blisters surrounded by red skin. Pustular psoriasis is often restricted to the palms or soles of the feet but occasionally can cover a large area of the body.
Erythrodermic psoriasis
Also known as exfoliative psoriasis, this type of psoriasis is the least common. This is a serious condition that requires immediate medical attention. It is characterised by a red, peeling rash across the entire body, which may burn or itch intensely. Erythrodermic psoriasis can be a side effect of severe sunburn or certain medications, such as oral corticosteroids. It may also occur if another type of existing psoriasis is poorly controlled.
Psoriatic arthritis
This painful inflammation of the lining of the joints is caused by the body's damaging immune response to psoriasis. Some estimates suggest that no more than one in five people with psoriasis will develop psoriatic arthritis. The severity differs from person to person, ranging from mild pain and swelling, right through to severe joint damage and disability in two out of five cases. In addition to the usual skin symptoms of psoriasis, psoriatic arthritis is characterised by pain, swelling and stiffness in one or more joints. There may also be pain and redness in the eyes and changes in the nails, such as thickening, discolouration and separation from the skin.
Generalised pustular psoriasis
Also known as von Zumbusch psoriasis, this rare condition is a serious form of pustular psoriasis. It is characterised by large areas of red skin that become painful and tender. Blisters usually form within hours of these initial symptoms and then dry over the next two days. As generalised pustular psoriasis is also accompanied by fever and a toxic reaction, hospitalisation is usually required for the administration of fluids and antibiotics through a drip.
Signs and symptoms
Psoriasis can range from a few patches of dandruff-like scaling to major outbreaks that cover large areas. The condition also varies in severity from being a mild inconvenience to being disfiguring, disabling and painful.
Symptoms tend to come and go, with the condition flaring for a few weeks to months, then fading or going into complete remission for some time. Psoriasis signs and symptoms vary between individuals, but usually include more than one of the following:
- Red patches of skin covered with silvery scales (plaques);
- Itching, burning or soreness;
- Dry, cracked skin that may bleed;
- Small, scaling spots (more commonly seen in children);
- Thickened, pitted or discoloured nails;
- Swollen and stiff joints;
- Inflammation of the eyelid or eyelid lining (conjunctivitis), and;
- Pain (especially in erythrodermic psoriasis, when plaques have been scratched, or in joints affected by psoriatic arthritis).
How do you stop psoriasis from spreading?
Preventing the spread of psoriasis involves adopting a comprehensive approach that addresses triggers, lifestyle factors, and proper skin care routines:
- Identify and Avoid Triggers: Pay attention to factors that trigger psoriasis flare-ups, such as stress, infections, skin injuries, and certain medications. Taking steps to minimise exposure to these triggers can help reduce the frequency and severity of symptoms.
- Maintain a Healthy Lifestyle: Adopting a healthy lifestyle can support overall well-being and may help manage psoriasis symptoms. This includes maintaining a balanced diet, staying hydrated, getting regular exercise, managing stress through relaxation techniques or therapy, and avoiding smoking and excessive alcohol consumption.
- Practise Good Skin Care: Proper skin care can help alleviate symptoms and prevent the spread of psoriasis lesions. This includes regularly moisturising the skin to prevent dryness and irritation, using gentle cleansers and avoiding harsh skincare products that may exacerbate symptoms.
- Seek Medical Treatment: Consult with a healthcare professional, such as a dermatologist, for personalised treatment recommendations tailored to your specific needs and symptoms. This may include topical treatments, phototherapy, oral medications, or biologic agents, depending on the severity and extent of psoriasis.
- Monitor and Manage Comorbidities (the presence of additional medical conditions that coexist with psoriasis): Individuals with psoriasis are at increased risk of developing other health conditions such as psoriatic arthritis, cardiovascular disease, and metabolic syndrome. Managing these comorbidities through regular medical check-ups, healthy lifestyle habits, and appropriate treatment is essential for overall health and well-being.
By adopting these strategies and working closely with healthcare professionals, individuals with psoriasis can effectively manage symptoms, prevent flare-ups, and improve their quality of life.
How can psoriasis be cured?
While psoriasis cannot be cured, various treatments are available to manage symptoms and improve quality of life. These may include:
- Topical Treatments: Topical corticosteroids, vitamin D analogues, retinoids, and calcineurin inhibitors are commonly used to reduce inflammation and slow skin cell turnover in psoriasis lesions.
- Phototherapy: Phototherapy, or light therapy, involves exposing the skin to ultraviolet (UV) light under medical supervision. UVB phototherapy and psoralen plus ultraviolet A (PUVA) therapy can help reduce inflammation and slow skin cell growth in psoriasis lesions.
- Oral Medications: Oral medications such as methotrexate, cyclosporine, and acitretin may be prescribed for moderate to severe psoriasis that does not respond to topical treatments or phototherapy.
- Biologic Agents: Biologic drugs, such as tumour necrosis factor (TNF) inhibitors, interleukin inhibitors, and phosphodiesterase-4 (PDE-4) inhibitors, target specific components of the immune system involved in psoriasis inflammation.
- Lifestyle Modifications: Adopting a healthy lifestyle, managing stress, maintaining a balanced diet, staying hydrated, getting regular exercise, avoiding smoking, and limiting alcohol consumption can help manage psoriasis symptoms and improve overall well-being.
While these treatments can effectively control symptoms and improve the quality of life for many individuals with psoriasis, it's essential to work closely with healthcare professionals to develop a personalised treatment plan tailored to your specific needs and preferences.
Is psoriasis a big deal?
Psoriasis is more than just a skin condition; it can have a significant impact on physical and emotional well-being. The visible nature of psoriasis lesions can lead to feelings of self-consciousness, embarrassment, and low self-esteem, affecting social interactions, relationships, and overall quality of life.
Furthermore, psoriasis is associated with an increased risk of developing other health conditions such as psoriatic arthritis, cardiovascular disease, metabolic syndrome, and depression. Managing these comorbidities through regular medical check-ups, healthy lifestyle habits, and appropriate treatment is essential for overall health and well-being.
While psoriasis cannot be cured, various treatments and management strategies are available to control symptoms, prevent flare-ups, and improve quality of life. By seeking medical treatment, adopting a healthy lifestyle, and prioritising self-care, individuals with psoriasis can effectively manage their condition and lead fulfilling lives.
Have you got more questions about your health? With Health&'s user-friendly personal health assistant, you can easily navigate through a series of simple questions to receive tailored support in just minutes.
Health& makes it easy to simply enter your search query in our A-Z library of medically verified health content, ensuring you find the best matches for your situation. Explore more health content, take early-intervention risk assessments, store your medical records and more! Discover the support you need with the Health& app, empowering you on your journey towards living better for longer.

