Colorectal cancer is the name for cancers that arise in the large intestine or rectum. Also known as colon cancer or colorectal cancer, bowel cancer can interfere with bowel function and spread to other parts of the body, such as the liver and lungs.…
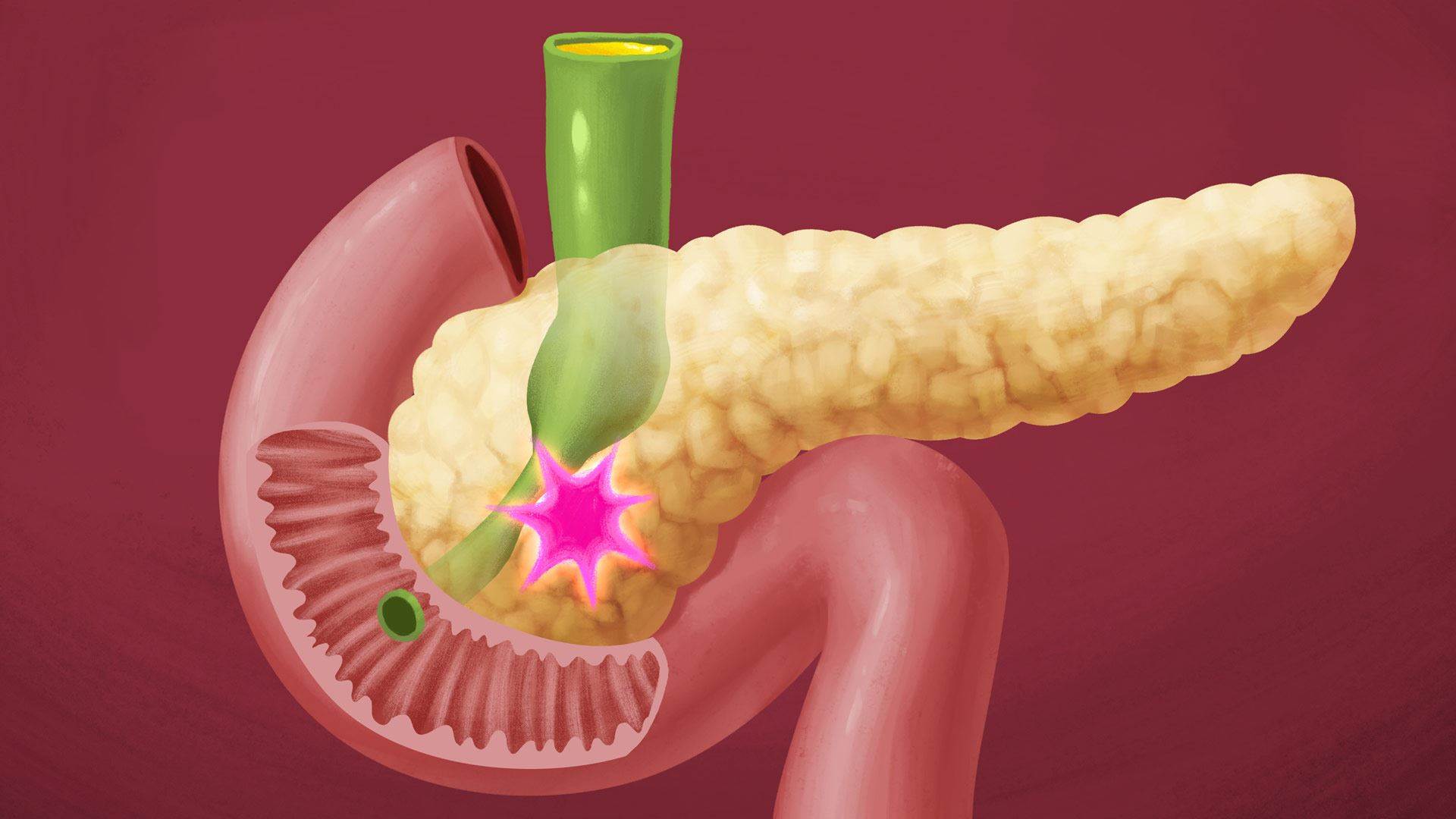
Pancreatic cancer
What is pancreatic cancer?
Pancreatic cancer occurs when abnormal cells grow uncontrollably in the pancreas, an organ located behind the stomach. The pancreas produces enzymes for digestion and hormones for blood glucose regulation.
These abnormal cells in the pancreas can grow to form a cancer, which can spread to other parts of the body.
Cells
The fundamental unit of life; the simplest living unit that can exist, grow, and reproduce independently. The human body is composed of trillions of cells of many kinds.
Glucose
A simple sugar found in many foods (such as fruit) that functions as a major energy source for the body.
Causes
The cause of pancreatic cancer, as with other cancers, is due to damage to cellular DNA. This damage results in uncontrolled growth of damaged cells, which leads to formation of a cancer. A cancer can grow into nearby tissue, or cells can break off and spread throughout the body via the bloodstream or lymphatic system. The exact causes of this cellular damage in the pancreas are not known.
 The pancreas and digestive system.
The pancreas and digestive system. Cells
The fundamental unit of life; the simplest living unit that can exist, grow, and reproduce independently. The human body is composed of trillions of cells of many kinds.
DNA
The genetic material of all living cells and some viruses. The full name is deoxyribonucleic acid.
Lymphatic system
A network of vessels, lymph nodes, the spleen and other organs that transport lymph fluid between tissues and bloodstream.
Risk factors
Risk factors that increase the chances of developing pancreatic cancer include:
- Smoking - it is associated with a two-to-threefold increase in the risk of developing pancreatic cancer;
- Age - people between 60-80 years of age account for more than 80% of cases;
- Chronic pancreatitis - inflammation of the pancreas is associated with cancer when it occurs over the long-term. The exact reason for this is unclear, but it is possible that prolonged inflammation causes damage to cellular DNA;
- Stomach surgery - the surgical removal of part of the stomach, due to a stomach ulcer or a cancer, is associated with an increased risk of developing pancreatic cancer, and;
- Diets high in meat, cholesterol and food preservatives.
DNA
The genetic material of all living cells and some viruses. The full name is deoxyribonucleic acid.
Inflammation
A body’s protective immune response to injury or infection. The accumulation of fluid, cells and proteins at the site of an infection or physical injury, resulting in swelling, heat, redness, pain and loss of function.
Types
Exocrine tumors
Exocrine tumors are the most common type of pancreatic cancer. They are cancers of the exocrine pancreas, which is where the exocrine glands are located. These glands produce the pancreatic enzymes that are released into the intestine.
Adenocarcinomas
Adenocarcinoma cancers form in the exocrine glands and account for about 95% of all exocrine pancreatic cancers.
Less common types of pancreatic cancers
There are several other types of exocrine cancers that form in areas around the exocrine glands rather than in the glands themselves.
Endocrine tumors
Endocrine tumors arise from the endocrine glands, originating in the cells that produce hormones. They are also called neuroendocrine tumors and are an uncommon type of pancreatic cancer. Endocrine tumors are defined as functional if they secrete hormones and non-functional if they do not.
Some types of endocrine tumors include:
- Insulinomas - originate in cells that produce insulin, the hormone that reduces blood glucose levels;
- Gastrinomas - originate in cells that make gastrin, a hormone that stimulates production of stomach acid;
- Glucagonomas - originate in alpha cells that produce glucagon, a hormone that raises blood glucose levels;
- Somatostatinomas - originate in cells that make somatostatin, a hormone involved in the regulation of other hormones;
- VIPomas - originate in cells that make vasoactive intestinal peptide, a neurotransmitter that has several regulatory functions, and;
- PPomas - originate in cells that produce pancreatic polypeptide, a hormone released in response to food ingestion.
 A cross-section of the pancreas showing the exocrine and endocrine glands.
A cross-section of the pancreas showing the exocrine and endocrine glands. Cells
The fundamental unit of life; the simplest living unit that can exist, grow, and reproduce independently. The human body is composed of trillions of cells of many kinds.
Endocrine
Of or relating to the body's endocrine glands, which secrete hormones into the bloodstream and surrounding tissues. This includes the pineal gland, pituitary gland, pancreas, ovaries, testes, thyroid, hypothalamus and adrenal glands.
Exocrine
Refers to the secretion of hormones and other substances out of a structure by way of a duct.
Glucose
A simple sugar found in many foods (such as fruit) that functions as a major energy source for the body.
Hormone
A chemical substance secreted in one part of an organism and transported to another part of that organism, where it has a specific effect.
Insulin
A hormone secreted by the pancreas in order to regulate glucose levels in the body's cells, which is used for energy.
Neurotransmitter
Chemicals that communicate signals from one nerve cell to another, or from nerve cells to other tissues.
Stages of pancreatic cancer
Treatment outcomes can vary greatly, depending on the stage of cancer. Cancer is staged according to its size and location, and whether it has spread to nearby or distant lymph nodes or organs throughout the body.
| Stage I | The cancer is located in the pancreas and has not spread. |
| Stage II | The cancer has spread to nearby lymph nodes or structures near the pancreas, but has not spread to other organs. |
| Stage III | The cancer has spread to nearby major arteries, with or without the lymph node being affected. |
| Stage IV | The cancer has spread to other organs such as the lungs or liver. |
Lymph node
A small organ of the lymphatic system containing many immune cells. Lymph nodes, also known as lymph glands, are the sites where many interactions between immune cells and foreign materials occur.
Signs and symptoms
Pancreatic cancer is uncommon and many of the following symptoms may also be due to other causes.
Jaundice and pale stools
If there is a blockage in a bile duct, it can cause jaundice, the symptoms of which include yellowing of the eyes and skin. It can also cause pale stools, if insufficient bile is present in the intestines to give stool its color.
Abdominal pain
Abdominal pain can occur when the pancreatic cancer irritates or invades surrounding nerves. Very rarely, it can be due to the cancer causing a bowel obstruction.
Nausea and vomiting
A blockage of the pancreatic or bile ducts can cause inflammation of the pancreas and put pressure on surrounding organs, which can lead to nausea and vomiting.
Loss of appetite and weight loss
Loss of appetite can be associated with nausea and vomiting. Weight loss can result from the cancer blocking the enzymes needed to digest food.
Unexpected onset of diabetes
Diabetes might develop if the cancer is disrupting the normal function of the pancreas. The pancreas produces insulin, a vital enzyme involved in sugar metabolism.
Bile
A fluid made in the liver and stored in the gall bladder.
Diabetes
A metabolic disorder that is caused by problems with insulin secretion and regulation and which is characterized by high blood sugar levels. Also known as diabetes mellitus.
Enzyme
Molecules (mainly proteins) produced by cells that can drive specific chemical reactions.
Inflammation
A body’s protective immune response to injury or infection. The accumulation of fluid, cells and proteins at the site of an infection or physical injury, resulting in swelling, heat, redness, pain and loss of function.
Insulin
A hormone secreted by the pancreas in order to regulate glucose levels in the body's cells, which is used for energy.
Intestines
The part of the digestive system from the stomach to the anus.
Abdominal
Relating to the abdomen, the middle portion of the trunk which contains organs such as the intestines, stomach and liver.
Methods for diagnosis
Scans
Scans used in the diagnosis of pancreatic cancer include:
- Computerized tomography (CT) scan - can help detect pancreatic cancer;
- Magnetic resonance imaging (MRI) - can provide detailed images of the pancreas, in particular the pancreatic duct, and;
- Positron emission tomography (PET) - can help to assess the tumor and its spread.
Laboratory tests
CA19.9 is a protein associated with pancreatic cancer, but its presence does not necessarily mean you have pancreatic cancer and it is not elevated in all forms of pancreatic cancer. It is mainly used to track the progress of treatment rather than to diagnose a tumor.
Pancreatic cancer can affect the function of the liver and kidneys, so tests are performed to check their functionality.
Procedures
Procedures performed to diagnose pancreatic cancer include:
- Endoscopy - involves the insertion of a long and narrow telescopic camera down the throat into the digestive system. This may be used to assess blocked pancreatic or bile ducts and reopen them with stents if possible;
- Laparoscopy - involves making a small incision in the abdomen so a camera can be inserted to see the internal organs. This may be done to determine the extent of the spread of pancreatic cancer and to do a biopsy, and;
- Tissue biopsy - involves removing a sample of pancreatic tissue for examination by a pathologist.
Abdomen
The part of the body that lies between the chest and the pelvis.
Bile
A fluid made in the liver and stored in the gall bladder.
Computerized tomography
A scan that uses X-rays to create a 3D image of the body. This can detect abnormalities more effectively than a simple X-ray can.
MRI
A type of imaging that uses a magnetic field and low-energy radio waves, instead of X-rays, to obtain images of organs.
Pathologist
A doctor specializing in the microscopic study of disease, such as examining a tissue sample taken in a biopsy.
PET
During positron emission tomography (PET) scan, an injection with a radioactive label is administered and then combined with a computerized tomography (CT) scan to produce functional images.
Stents
Small mesh tubes made of metal or plastic, which are inserted into passageways that are blocked or obstructed.
Tumor
A growth caused by an abnormal and uncontrolled reproduction of cells.
Types of treatment
Surgery
Surgery is used to remove a cancer that has not spread. If you have pancreatic cancer and are fit for major surgery, your doctor will perform a procedure called Whipple's resection. This is where a portion of the gall bladder, bile ducts and sometimes stomach are removed.
Another type of procedure, called a distal pancreatectomy, involves removing the cancer and surrounding tissue from the tail end of the pancreas. If the cancer cannot be removed, other forms of surgery can be used as a means of relieving symptoms. For example, stents can be inserted into the bile and pancreatic ducts to keep them open.
Additional therapy
Other therapies can be used in addition to surgical treatments to further improve treatment outcomes. They may be given before surgery (neoadjuvant therapy) and/or after surgery (adjuvant therapy). When given before surgery, they aim to reduce the size, and therefore stage, of the cancer. When given after surgery, they aim to help prevent the cancer returning. These non-surgical treatments include chemotherapy, radiotherapy, hormone therapy or a combination of these.
Occasionally, these therapies may be used if individuals are not suitable for surgical treatment. Often, in these situations, the aim of treatment is to control symptoms, and are not necessarily for cure. The treatment options and aims can differ, based upon the individual, the stage and type of cancer. Your doctor can help explain this information in more detail.
Chemotherapy
Chemotherapy works by damaging cancer cells and stopping their reproduction. Various medications can be used, which can be administered intravenously or orally. They are often given in cycles, with intervening rest periods, to help reduce toxic side effects.
Side effects occur because chemotherapy can also affect healthy cells. Your doctor will monitor your dosage carefully to achieve the best therapeutic effect.
Radiotherapy
Radiotherapy focuses X-rays on the area where the cancer is located. Radiotherapy can be used alone, or in addition to surgery and/or chemotherapy.
Hormone therapy
Hormone therapy is sometimes used to treat advanced pancreatic cancer, if the cancer cells are found to carry a particular hormone receptor. For example, some pancreatic cancers have estrogen receptors and tamoxifen is a medication that can be used to block that receptor, potentially slowing the growth of the tumor.
Other therapies
Some people diagnosed with cancer seek out complementary and alternative therapies. None of these therapies are proven to cure cancer, but some can help people feel better when used together with conventional medical treatment. It is important to discuss any additional treatments with your doctor before starting them.
Bile
A fluid made in the liver and stored in the gall bladder.
Cells
The fundamental unit of life; the simplest living unit that can exist, grow, and reproduce independently. The human body is composed of trillions of cells of many kinds.
Gall bladder
A small organ attached to the liver that stores bile until it is released into the small intestine, to aid the digestion of food.
Hormone
A chemical substance secreted in one part of an organism and transported to another part of that organism, where it has a specific effect.
Intravenously
Within a vein.
Stents
Small mesh tubes made of metal or plastic, which are inserted into passageways that are blocked or obstructed.
Tumor
A growth caused by an abnormal and uncontrolled reproduction of cells.
Potential complications
Treatment side effects
Side effects of treatment for pancreatic cancer can include:
- Nausea, vomiting and fatigue;
- Altered bowel habits, such as constipation or diarrhea;
- Joint and muscle pain;
- Temporary hair loss from the head and body, and;
- Tingling in the hands and feet - some chemotherapeutic agents can affect the nerves. It is important to tell your doctor if you develop these symptoms.
Advanced pancreatic cancer
Metastasis is when the cancer spreads to other parts of the body through the bloodstream and lymphatic system. The metastasized cancer damages the function of an affected organ or body part.
Bowel obstruction
If the pancreatic cancer grows and puts pressure on the small intestine, it can cause a bowel obstruction or blockage, which reduces the flow of food from the stomach to the intestines.
Intestines
The part of the digestive system from the stomach to the anus.
Lymphatic system
A network of vessels, lymph nodes, the spleen and other organs that transport lymph fluid between tissues and bloodstream.
Prognosis
The outlook for pancreatic cancer depends on the type and stage of cancer, however the overall survival rates are usually low, as it is most often diagnosed at an advanced stage.
It is important to remember survival rates are only an indication, and are based upon the averages of previously treated patients. It is not an absolute prognosis for an individual. It is often difficult to accurately predict an individual's cure or survival rate. Constant advances in treatment are continually improving these statistics.
As pancreatic cancer progresses, the aim of treatment shifts from extending life to minimizing pain, with palliative care available for terminal patients.
Palliative care
The comprehensive care of unwell and terminally-ill patients that is aimed at making them as comfortable as possible, rather than prolonging their life. It includes pain management, counselling, education and support for their family/carers.
Prevention
Maintaining a healthy weight, quitting smoking and avoiding alcohol overuse are the best means of reducing your risk of pancreatic cancer.






